Built to upscale your RCM
Automated Revenue Cycle Platform for Care Providers
AI-powered, program-aware revenue agents built on the Anise clearinghouse, orchestrating billing, claims, and payments with precision and scale.
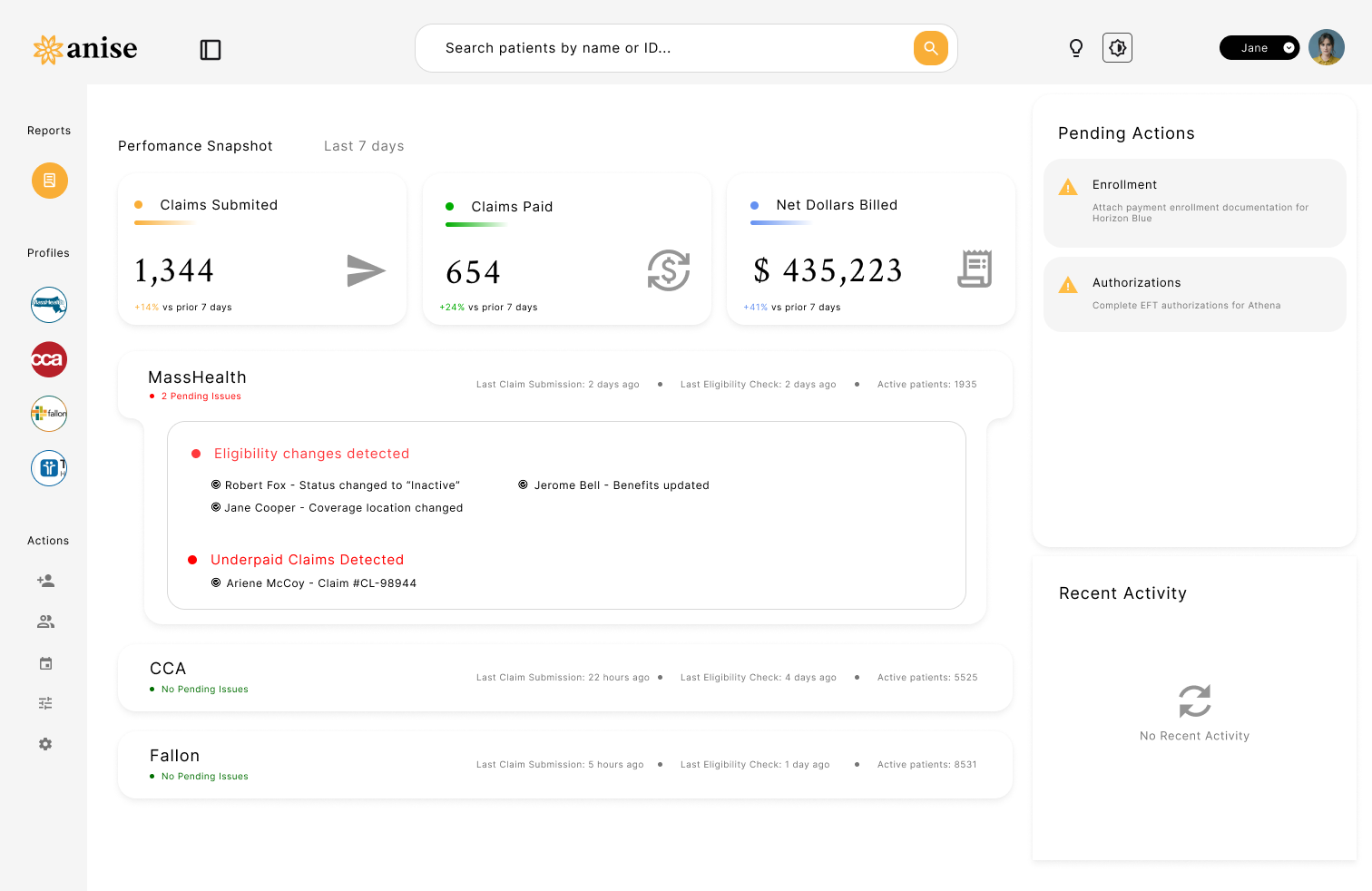
How Anise supercharges your RCM motions
Anise automates eligibility checks, authorization tracking, claim submission, and payment reconciliation.

Validate program rules before claims go out
Anise checks payer and program requirements early so your team catches issues before submission.
Monitor eligibility and authorizations continuously
Stay ahead of coverage changes, expiring authorizations, and missing units before they delay care or payment.

Run billing on a reliable schedule
Automate claim submissions and status checks on the billing cadence your team already uses.

Reconcile payments and report in real time
Track what is paid, what is pending, and what needs action without waiting for end-of-month cleanup.

Validate program rules before claims go out
Anise checks program parameters and payer requirements before submission, so your team catches errors earlier and submits cleaner claims.
Monitor eligibility and authorizations continuously
Agents verify eligibility and authorized units throughout the cycle to reduce denials and avoid billing delays.
Run billing on a reliable schedule
Automate claim submissions and status checks on pre-set billing cycles so your team keeps cash flow moving without manual follow-up.
Reconcile payments and report in real time
Get clear reporting across claims and payments with traceable revenue activity and fewer surprises at month end.
Connected to major payer and state program networks
Direct connectivity helps your team spend less time chasing status updates and more time fixing issues that matter.
Revenue visibility without guesswork
Anise does not hide decisions behind a black box. Teams see what changed, why it matters, and what to do next.
Claim risk alerts
Flag likely denials before submission so staff can correct issues early.
Eligibility monitoring
Detect coverage changes before they create avoidable denials or service interruptions.
Authorization tracking
Catch expiring, missing, or underused authorizations before billing is blocked.
Payment reconciliation
Track paid, pending, and mismatched payments without spreadsheet cleanup.
Why teams choose Anise
Built for healthcare billing workflows, connected directly to payer networks, and designed so your team keeps control over rules and approvals.
Request a demoProgram-specific billing support
Built for AFC, GAFC, home health, and skilled and unskilled nursing workflows.
Direct payer connectivity
Real-time claim status and fewer handoffs through your own clearinghouse layer.
Automation with approvals
Automate repetitive work while keeping review steps, rules, and audit trails.
Trusted by teams that need billing to run on time
Having billing handled end to end changed our day-to-day work. Eligibility checks, prior auth tracking, and claim submission are finally consistent.
Operations Director
Post-acute provider
Prior authorizations are predictable now. We fix issues before they become denials.
Billing Operations Lead
Community care provider
Denial trends are visible early, so our team spends less time guessing and more time resolving.
Revenue Cycle Manager
Home health organization
Payments are reconciled daily, and we always know what is pending and what needs follow-up.
Finance Director
Multi-site provider group
CEO's Desk quote
"Built to run your revenue cycle.
You focus on care."
See what billing looks like when the workflow is built for healthcare
Get a walkthrough of eligibility checks, claim automation, and reconciliation built around your billing process.
Request a demo