A platform for billing operations
The payments engine behind modern care delivery
Anise helps your team validate claims, monitor coverage, track authorizations, and reconcile payments in one workflow built for healthcare billing.
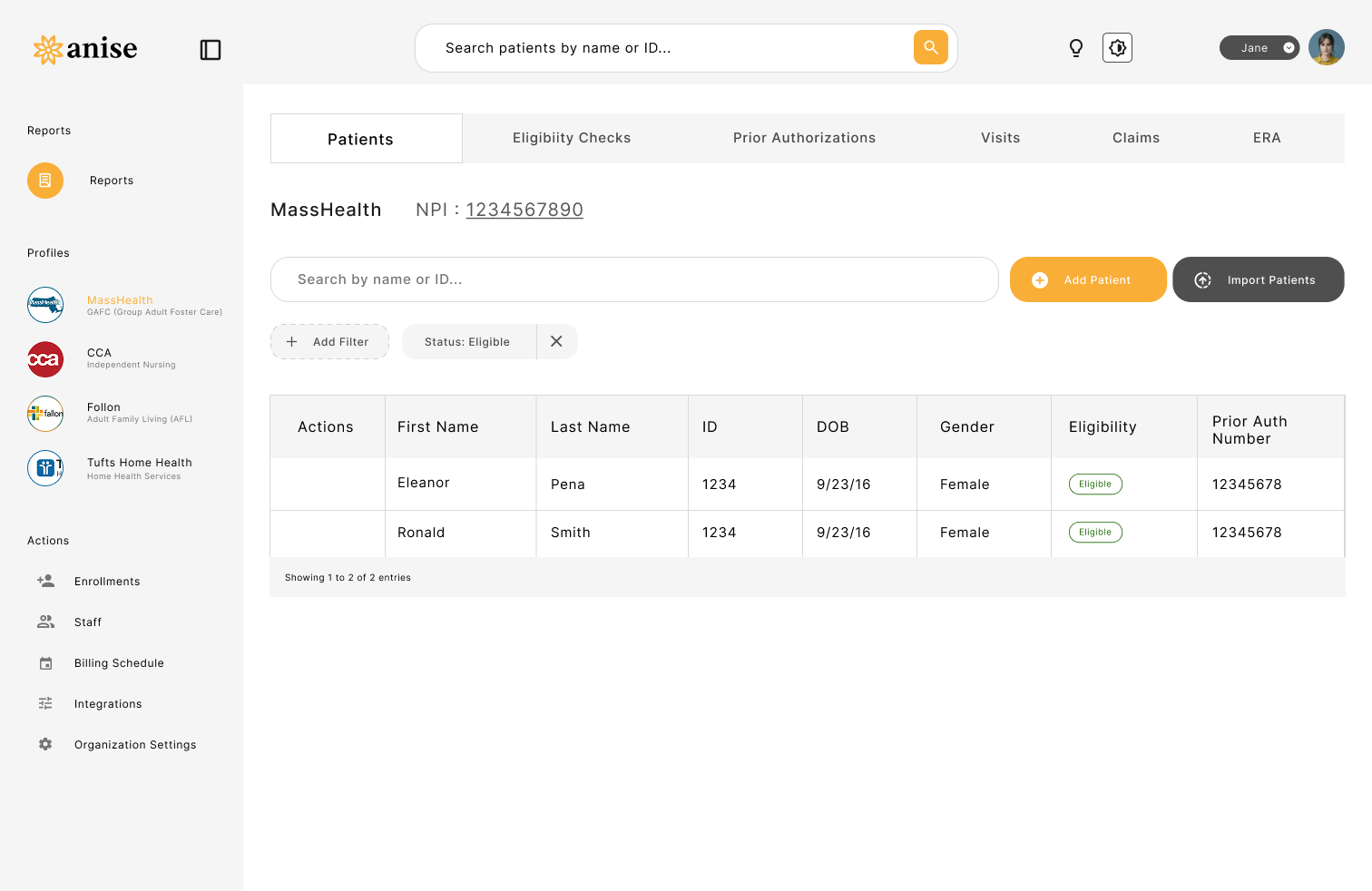
Automated healthcare billing workflows
Move from manual follow-up to a predictable billing process.
Real-time claim status
See what is pending, paid, or blocked so your team can act faster.
Operational lift
Less rework
Designed to reduce repetitive tasks across the billing cycle.
Transaction tracking with full visibility
Trace claims and payments from submission through reconciliation.
Built for the full billing cycle
Anise is designed to support the actual flow of work across eligibility, authorizations, claims, and payments, so teams do not have to stitch together updates across tools.
See Anise on your workflow
Get a walkthrough based on your billing process, payer mix, and current blockers.
Everything your billing team needs to keep revenue moving
Each feature is designed to prevent avoidable denials, shorten follow-up cycles, and improve day-to-day operational clarity.
Eligibility monitoring before billing issues become denials
- Continuous eligibility and benefits checks across active patients
- Alerts for coverage changes before claim submission
- Daily monitoring that reduces manual lookups and missed updates

Authorization tracking that keeps billing on schedule
- Prior authorization ingestion and status tracking
- Expiration and renewal alerts so teams can act early
- Clear visibility into missing or expiring authorizations

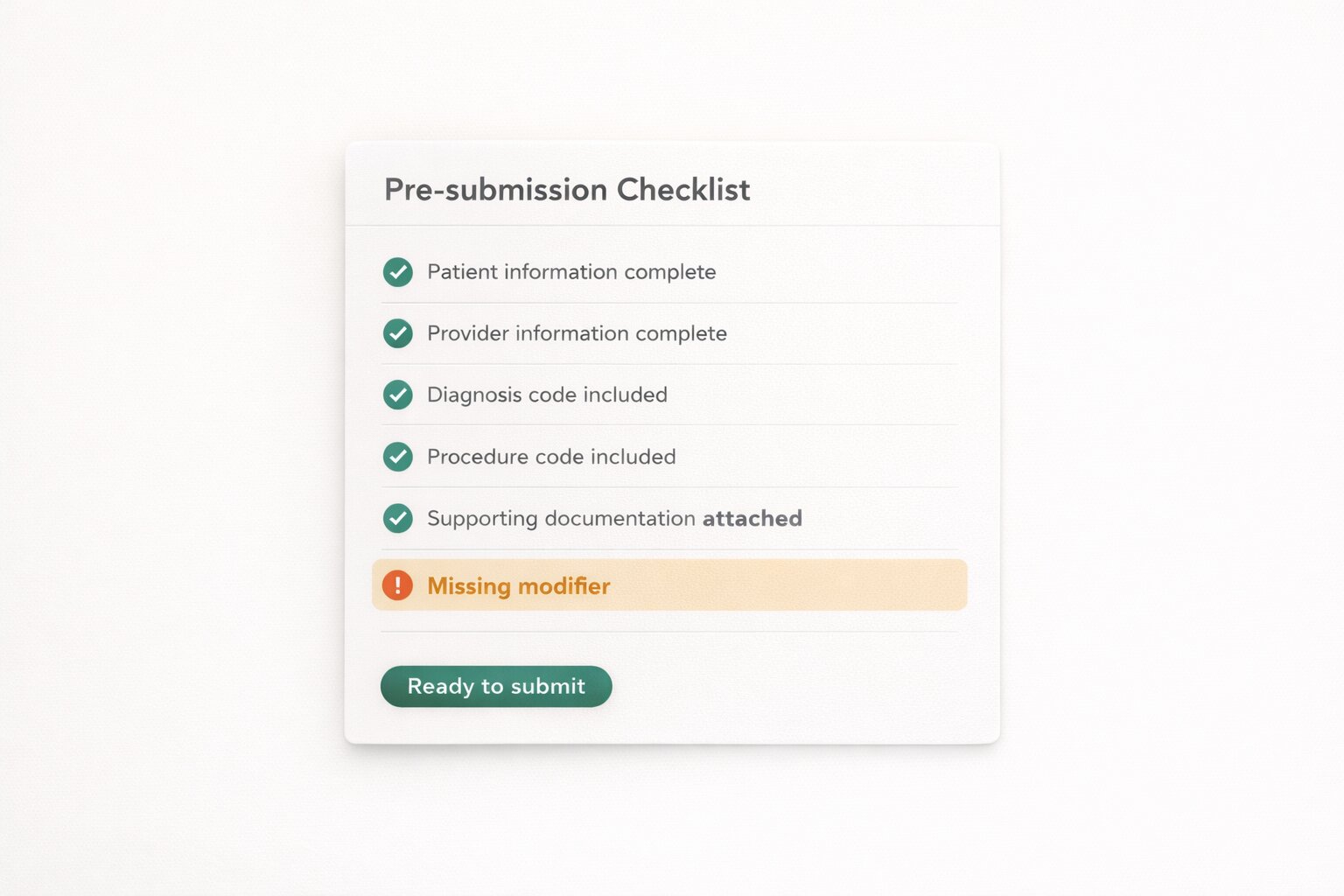
Claim automation with validation before submission
- Program-specific claim generation for healthcare workflows
- Pre-submission checks to reduce preventable denials
- Claim status tracking and rebilling workflows in one system
- Direct payer connectivity for faster processing visibility
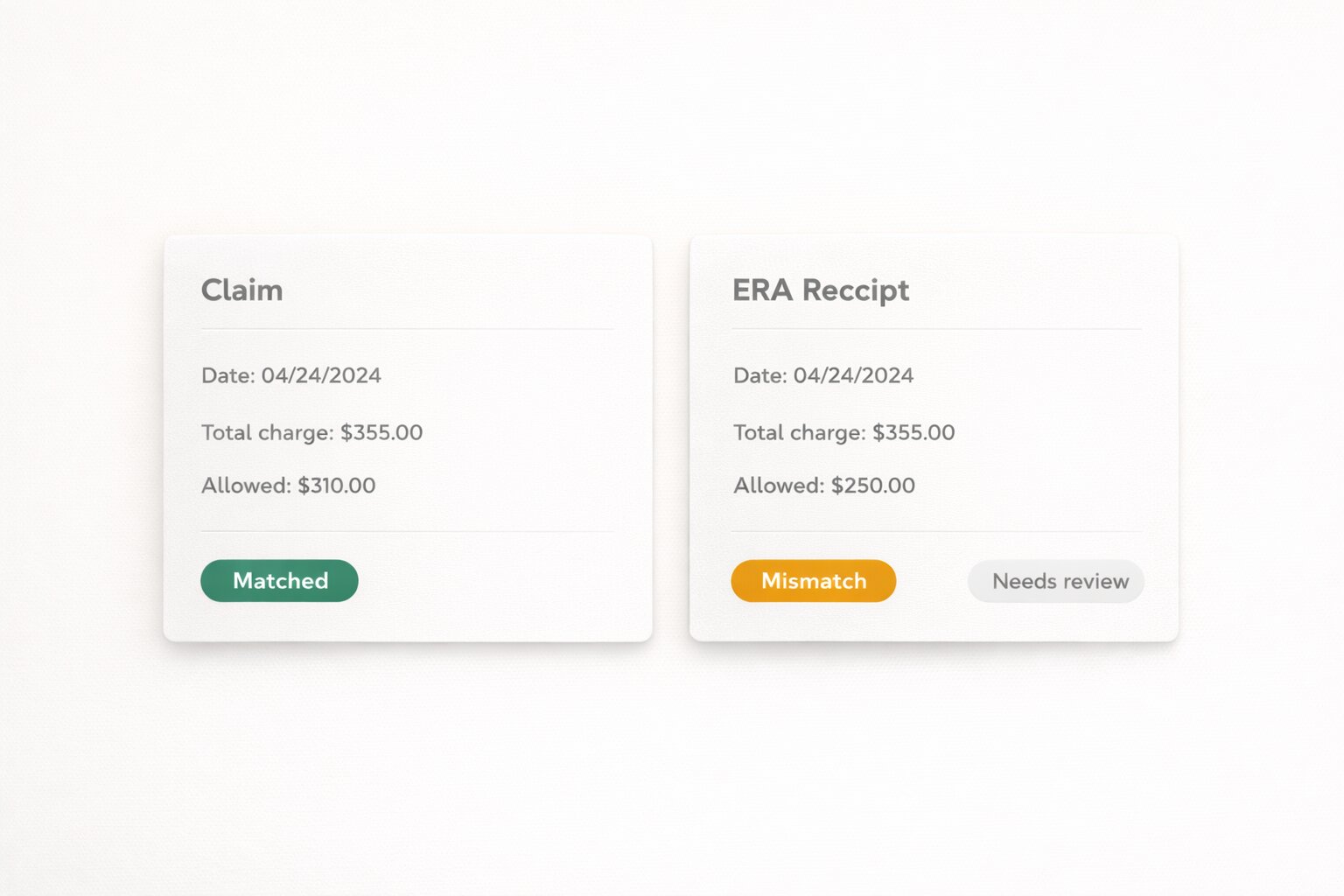
Payment reconciliation that gives finance teams clarity
- ERA ingestion and automated reconciliation workflows
- Visibility into paid, pending, and mismatched transactions
- Less manual payment follow-up and cleaner month-end review
Reporting your team can use every day
- Track claims and payments from submission to reconciliation
- Monitor denial patterns, reimbursements, and bottlenecks
- Support faster decisions with clear operational reporting

Tools that reduce manual work and improve billing outcomes
Streamlined payment management
Track payment status and reconciliation without spreadsheet cleanup.
- ERA reconciliation visibility
- Fewer unmatched payments
Billing automation
Automate repetitive billing steps while keeping rules and approvals in place.
- Consistent billing cycles
- Less manual follow-up
Access control and configuration
Role-based permissions and workflow controls help teams reduce mistakes.
- Role-based permissions
- Configurable rules and approvals
Proactive revenue intelligence
Identify billing risks early with visibility into eligibility, auths, and claim status.
- Denial risk signals
- Coverage drift alerts
Seamless EHR integrations
Keep patient and billing data aligned across systems with built-in sync.
- Cleaner patient context
- Fewer duplicate entries
One workflow, one source of truth
From eligibility checks to payment reconciliation, your team works in one system.
How teams get started with Anise
A practical rollout that connects systems, enrolls payers, and validates billing before go-live.
Connect your EHR
Sync patient and billing data so records stay aligned from the start.
Enroll payers
Complete credentialing and enrollment so you can submit claims without delays.
Go live and validate
Launch with confidence and validate early transactions before scaling volume.
Get live without disrupting current operations. We help teams move step by step and validate early results.
Request a demoSecurity and reliability built into every transaction
Anise is designed for healthcare billing operations with controls, encryption, and monitored systems that support production use.
Compliance
- HIPAA-aligned operational practices
- Clear auditability across billing actions
Security
- Encryption in transit and at rest
- Role-based access and permission controls
Reliability
- Monitored billing and transaction pipelines
- Redundant infrastructure for production uptime
Want to see how this applies to your billing workflow?
We can walk through your current process and show where Anise helps first.